Bizarre medical treatments people once believed in
Before antibiotics and lab tests, many healers worked from the humoral playbook championed by Hippocrates and Galen. If illness was an imbalance of blood, phlegm, black bile, and yellow bile, then bleeding, purging, and sweating felt logical. Barber-surgeons set bones and opened veins; apothecaries dispensed draughts spiked with herbs, metals, and resins. Folk remedies mingled with learned medicine, and the line between cure and spectacle could be thin.
That began to shift in the 1800s with anesthesia, statistics, and germ theory. Louis Pasteur’s experiments in the 1860s and Robert Koch’s bacteria identifications in the 1880s reframed disease. Regulation slowly followed: the US Pure Food and Drugs Act of 1906 attacked misbranding, and the 1938 Food, Drug, and Cosmetic Act demanded safety data. Not every fad disappeared overnight, but the age of evidence started elbowing out the age of elixirs.
Bloodletting and leeches: when losing pints meant gaining health

For centuries, doctors reached for lancets as readily as stethoscopes. Bloodletting was prescribed for fevers, headaches, even melancholy, all to lighten an overloaded circulatory system. The most famous cautionary tale is George Washington, who in December 1799 was bled about 80 ounces of blood in less than a day while ill with a throat infection. That is roughly 2.4 liters, around a third of an adult’s blood volume, and he died soon after.
Leeches made the practice look tidier.
The European medicinal leech, Hirudo medicinalis, boomed in the 1800s, with France alone importing millions annually. Odd twist: leeches earned a second life in modern operating rooms. In 2004, the US Food and Drug Administration cleared them as medical devices to relieve venous congestion after microsurgery, where their anticoagulant saliva and steady sipping can salvage reattached ears, fingers, and fragile skin flaps.
Trepanation: opening your mind the hard way
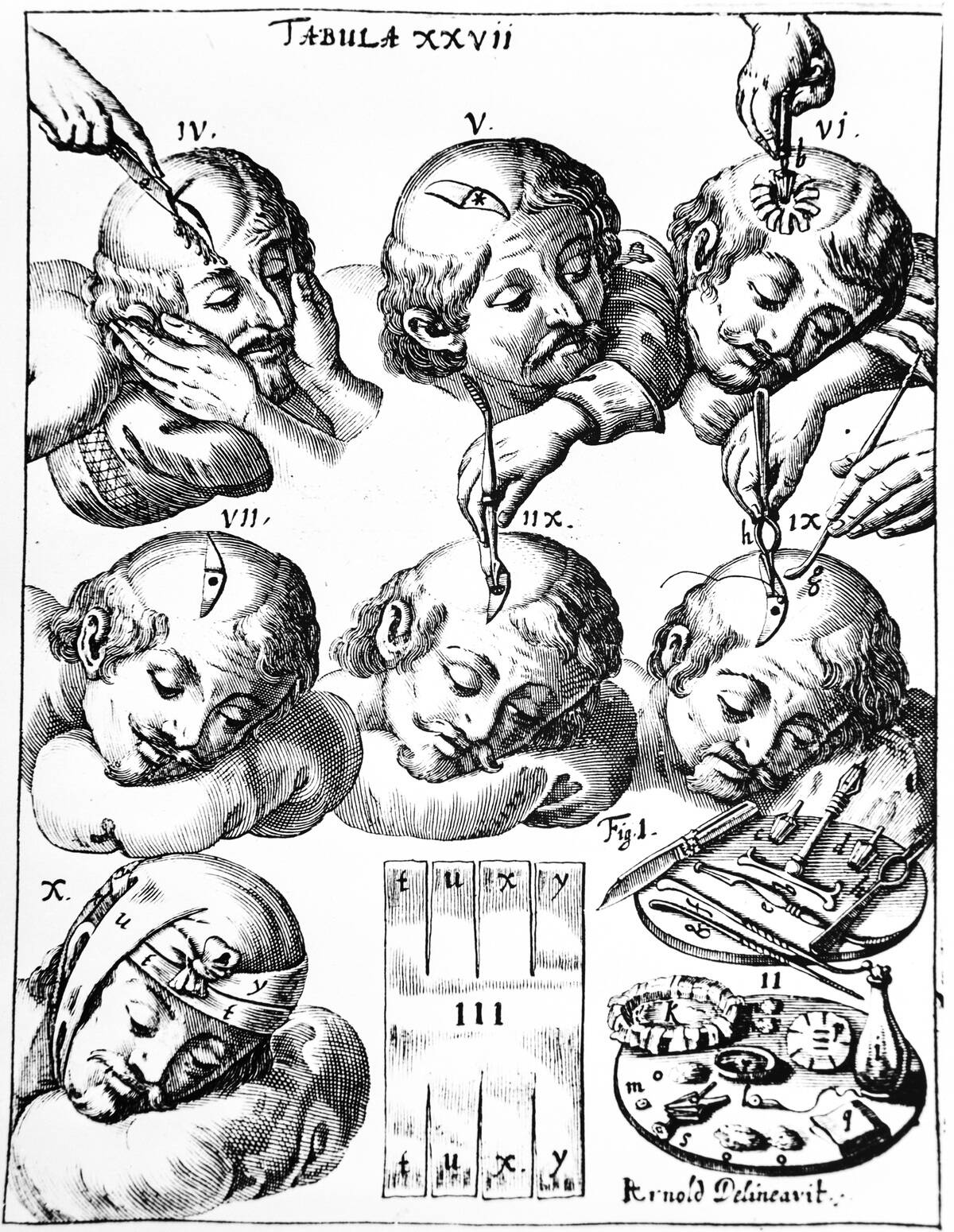
Archaeologists find skulls from Neolithic Europe and pre-Columbian Peru bearing careful round holes, with bony smoothing that shows many patients survived. These trepanations likely addressed head trauma, seizures, or spiritual concerns, accomplished with stone tools long before steel. In Peru, survival rates appear to have improved over centuries, suggesting technique mattered even without germ theory or anesthesia.
Later surgeons kept the idea but refined the tools. Renaissance master Ambroise Paré described trephines to relieve pressure after skull fractures. Today, craniotomies still open the skull for hemorrhages and tumors, but with asepsis, imaging, and neuroanesthesia steering the way. The old instinct that pressure inside the head can be deadly was right; the hand-cranked execution, less so.
Mercury and arsenic tonics: poison as panacea

For generations, syphilis met its match in mercury ointments and vapors, spawning the bleak quip: a night with Venus, a lifetime with Mercury. Calomel, a mercurous chloride laxative, was a 19th-century staple championed by physician Benjamin Rush; it purged mightily and poisoned quietly. Mercury’s neurotoxic and renal harms were not fully appreciated, even as tremors and tooth loss hinted loudly at trouble.
Arsenic had an equally strange double life. Fowler’s solution, a potassium arsenite tonic introduced in 1786, treated psoriasis and anemia, and was sipped into the early 1900s. Then came a breakthrough that bridged poison and precision: in 1909–1910, Paul Ehrlich’s arsphenamine (Salvarsan), an arsenic-based compound, provided the first effective antimicrobial therapy against syphilis. It worked better than mercury but still carried risks, foreshadowing the safer antibiotic era.
Laudanum and opium: the Victorian cure-all in a bottle

Laudanum, a tincture of opium in alcohol popularized by Thomas Sydenham in the 17th century, became the Victorian nightcap for pain, coughs, diarrhea, and grief. Apothecaries sold it freely, and patent nostrums like Godfrey’s Cordial and Mrs. Winslow’s Soothing Syrup dosed even infants. Writers such as Thomas De Quincey and Samuel Taylor Coleridge documented its seductive relief and heavy costs in the 1800s.
Rules arrived unevenly.
Britain’s Pharmacy Act of 1868 restricted sale of many poisons, including opium, to registered chemists. In the United States, the Pure Food and Drugs Act of 1906 mandated labeling of narcotic content, and the Harrison Narcotics Tax Act of 1914 tightened control. As addiction and overdose became harder to ignore, the era of opiated everything ebbed, though the clinical power of morphine and codeine remained.
Mummy powder (mumia): a spoonful of pharaoh for what ails you

Early modern Europe swallowed a startling prescription: ground-up mummified remains. Apothecaries stocked mumia as a hemostatic and tonic, confusing the original Arabic term for bitumen with Egyptian mummies themselves. Thinkers from Paracelsus to Francis Bacon mentioned mumia in their medical musings, and jars of the stuff traveled from Cairo markets to Paris and London shop shelves.
Demand bred deception. In 1564, French physician Guy de la Fontaine reported that many so-called mummies sold to Europeans were recently prepared corpses, darkened with pitch. The idea also bled into art: a pigment dubbed mummy brown, made from funeral remains, was used into the 19th century before squeamishness and skepticism finally shuttered the trade. The romantic aura of antiquity did not equal efficacy.
Tobacco smoke enemas: blowing smoke where the sun doesn’t shine
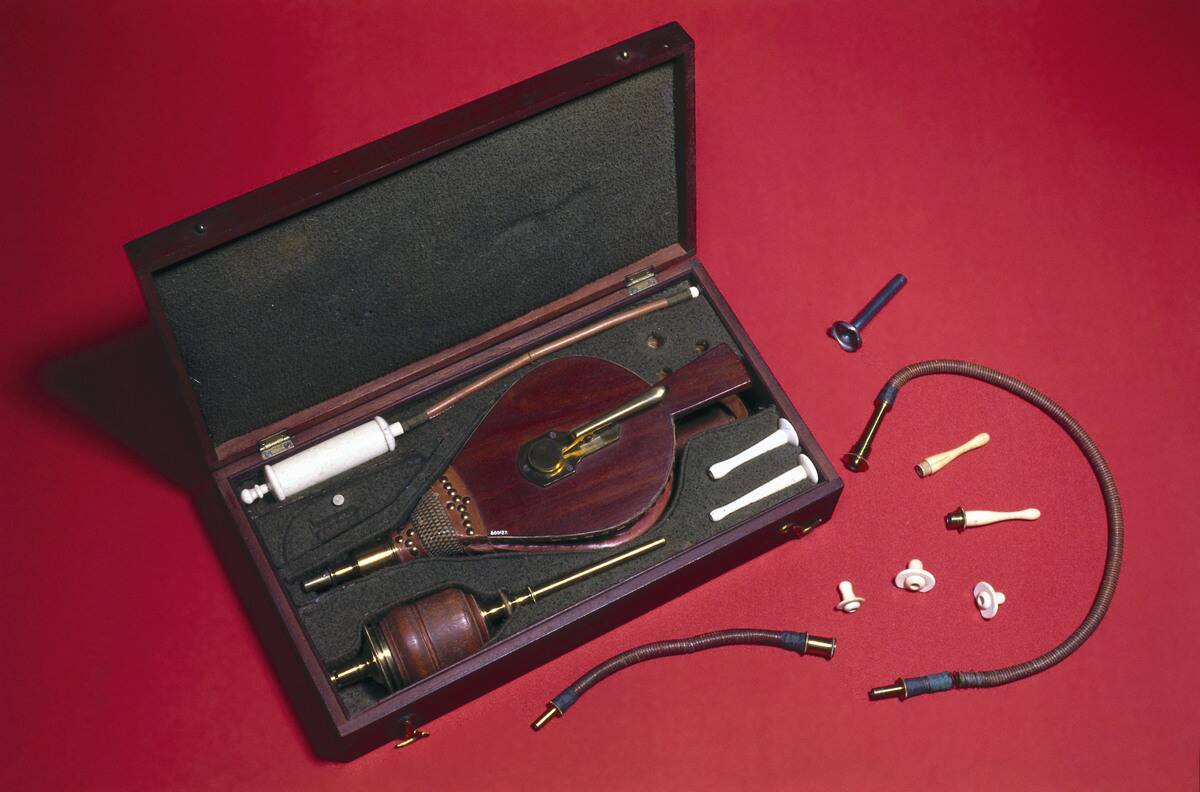
In the late 1700s, lifesaving kits along the River Thames included bellows for tobacco smoke enemas. The Royal Humane Society, founded in 1774 to promote resuscitation, endorsed the practice for drowning victims, colds, and more. The logic flowed from then-fashionable ideas about stimulating the body and warming the bowels back to life.
As physiology advanced, the practice deflated. Nicotine’s toxicity, coupled with lack of evidence, saw smoke bellows fall from favor by the early 19th century. Mouth-to-mouth and, much later, chest compressions delivered better odds. It is a rare case where the idiom and the intervention both aged poorly.
Radium water and glow-up wellness

When Marie and Pierre Curie’s discoveries electrified the 1900s, entrepreneurs bottled the buzz. Radithor, a radium-226 and radium-228 laced water made by William J. A. Bailey, promised vigor. Industrialist Eben Byers reportedly drank hundreds of bottles; he died in 1932 with devastating bone damage. Regulators took notice, and the Federal Trade Commission moved against such radioactive panaceas.
The human toll extended beyond luxury decanters. The Radium Girls, dial painters who licked their brushes for fine points in the 1910s and 1920s, developed jaw necrosis and cancers. Their lawsuits helped shape industrial safety standards. The era’s radiance sold well, but the physics of alpha emitters and bone-seeking elements made the risks painfully literal.
Cocaine toothache drops and heroin cough syrups

Cocaine’s legitimate medical debut came in 1884 when ophthalmologist Carl Koller showed its value as a local anesthetic. Soon, companies peddled cocaine toothache drops over the counter; period ads from firms like Lloyd Manufacturing promised quick relief for kids and adults alike. The numbing worked, but dependence and toxicity were never far behind.
Heroin, synthesized by Bayer chemists in 1898 as diacetylmorphine, was marketed as a smoother, supposedly non-addictive cough suppressant for bronchitis and tuberculosis. That claim did not survive clinical experience. The United States tightened narcotics control with the Harrison Act in 1914 and banned heroin for nonmedical use in 1924, as doctors pivoted toward safer, evidence-backed treatments.
Snake oil and patent medicines with magical labels

Nineteenth-century patent medicines rarely held patents; they traded on branding and secrecy. Many were heavy on alcohol, caffeine, or opiates. Lydia Pinkham’s Vegetable Compound, for example, offered women relief with a generous ethanol assist, while other tonics promised renewed manhood or preserved youth in flowery prose and fine print.
Snake oil became the symbol of it all.
In 1916, a federal case showed Clark Stanley’s Snake Oil Liniment contained no snake derivative, only mineral oil, chili, and turpentine. The 1906 Pure Food and Drugs Act armed authorities against misbranding, and truth-in-advertising slowly nudged the market from miracle toward measurable.
The royal touch for scrofula: healing by divine right
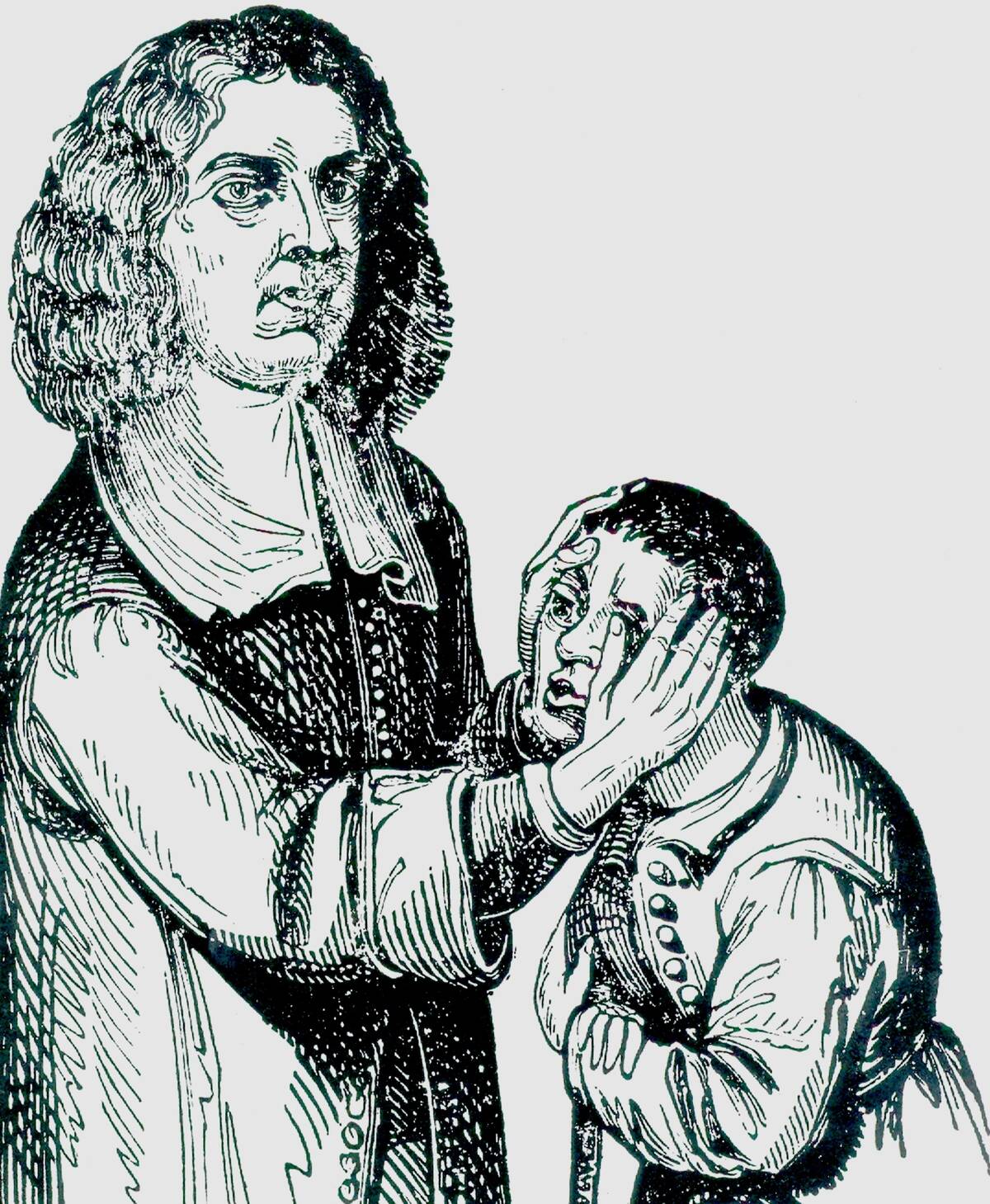
For medieval and early modern subjects, a king’s fingers seemed medicinal. English and French monarchs laid hands on people with scrofula, a form of tuberculous lymph node disease, in ceremonies that fused politics and piety. Chronicles trace the English rite to Edward the Confessor in the 11th century, while French kings cultivated a parallel tradition.
The practice persisted astonishingly long.
Queen Anne was the last British monarch to touch for scrofula, in 1712; among those presented as a child was Samuel Johnson, later famed lexicographer. As Enlightenment skepticism and modern medicine spread, the ritual dimmed, leaving a curious footnote on the placebo power of pageantry.
Plague doctor beak masks and posies against “bad air”

The iconic beak mask likely traces to Charles de Lorme, physician to Louis XIII, who in 1619 described a waxed coat, glass goggles, and a beak stuffed with aromatics like myrrh and mint. A cane kept patients at a distance. It was a practical response to a wrong idea: that sweet scents could filter or counteract deadly miasmas.
During outbreaks like the Great Plague of London in 1665, people clutched pomanders and posies, splashed vinegar, and shuttered homes. Unfortunately, Yersinia pestis rode on fleas and rats, indifferent to perfume. While quarantine and flight sometimes worked, the beak mask is a striking relic of the era’s olfactory defenses.
Phrenology: reading head bumps for health and habits
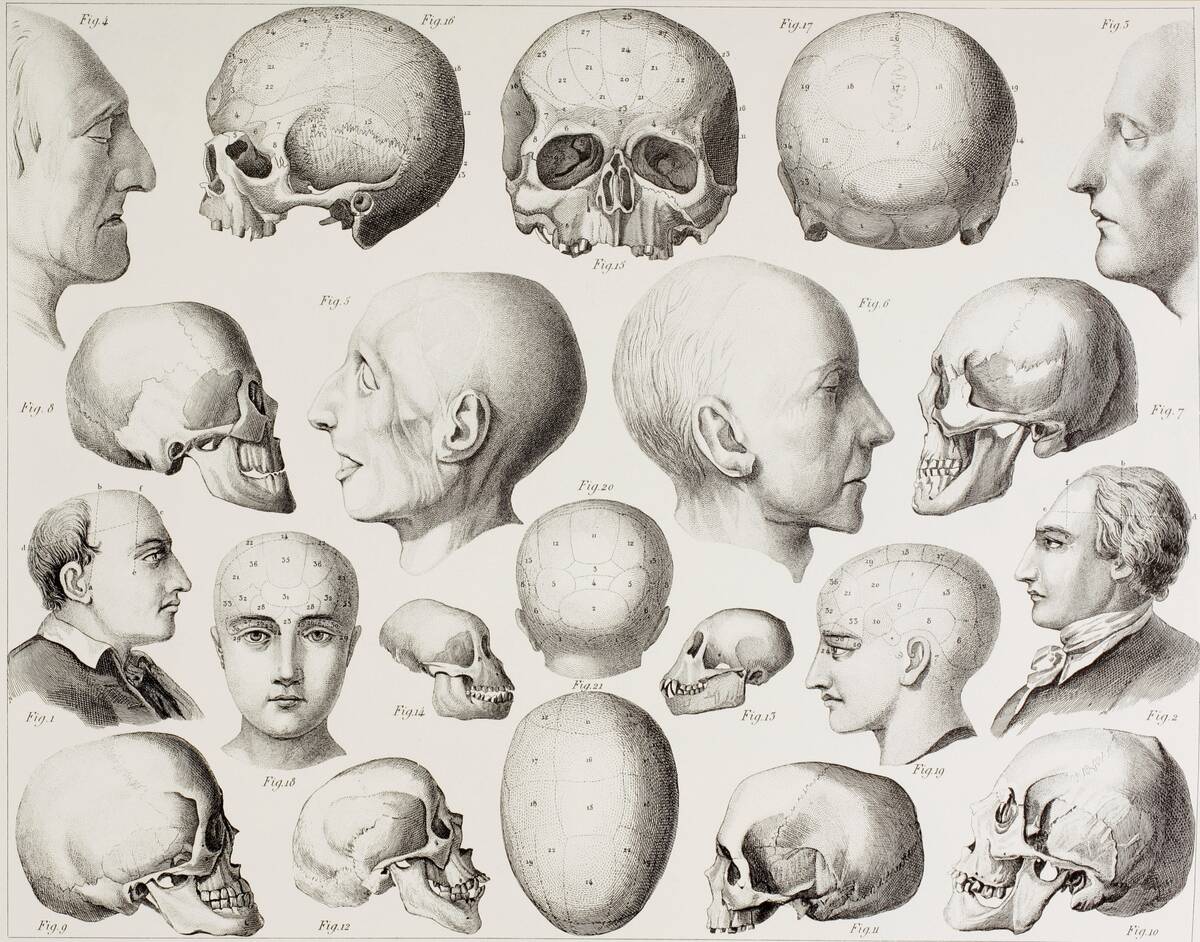
In the early 1800s, Franz Joseph Gall proposed that mental faculties mapped to brain regions whose growth subtly shaped the skull. Johann Spurzheim popularized the idea, spawning parlors where practitioners palpated bumps and charted character. In New York, Fowler and Wells ran a bustling phrenological cabinet and journal, bringing cranial cartography to the masses.
It seeped into hiring, education, and prison classification. But as neurology advanced, the cranial map unraveled. By the late 19th century, empirical studies and improved anatomy showed skull contours did not mirror personality. Still, phrenology’s clumsy localization arguably nudged scientists toward investigating specialized brain functions with rigor.
Mesmerism and animal magnetism: you are getting very healthy…

Franz Anton Mesmer claimed in the 1770s that an invisible fluid, animal magnetism, coursed through living things and could be redirected to heal. Parisian salons filled with crises and cures. In 1784, a royal commission including Benjamin Franklin and Antoine Lavoisier concluded the effects were due to imagination and suggestion, not a physical force.
The show did not end there.
Mesmeric demonstrations evolved into stage acts, while physicians like James Braid in the 1840s reframed the practice as hypnotism with psychological mechanisms. Surgeons such as James Esdaile reported operating with mesmeric anesthesia in colonial India, though results and interpretations remain debated. The mind’s role in healing grew harder to dismiss.
Victorian “hysteria” and the rise of the medical vibrator

Victorian doctors diagnosed many women with hysteria, a catchall for symptoms from pain to anxiety. Pelvic massage appeared in some case notes, but the oft-repeated tale of exhausted physicians mechanizing the task is more pop-culture than proof. Joseph Mortimer Granville’s 1880s mechanical percussor, for instance, was designed for muscle therapy, not hysteria.
What is certain: electric home massagers arrived early.
Hamilton Beach patented a handheld electric vibrator in 1902, and by the 1910s–1920s, vibrating appliances filled mail-order catalogs as tonics for nerves, circulation, and aches. Meanwhile, psychiatry’s vocabulary shifted, with psychoanalytic theories and later diagnostic manuals retiring hysteria as a medical label.
Blistering, cupping, and cantharides: raise a welt, chase a fever

Counterirritation once promised to draw out disease by drawing the skin. Spanish fly, the beetle Lytta vesicatoria, yields cantharidin, a potent blistering agent used for fevers and rheumatism. It also causes painful urinary irritation and dangerous toxicity, making its parallel life as an aphrodisiac notorious for poisonings rather than romance.
Cupping marks dot athletes today, but the method is ancient. Heated cups or suction create bruising circles; wet cupping adds scarification and bloodletting. Western doctors used cupping in the 18th and 19th centuries, and it remains in traditional medicine. A modern twist: in 2023, the FDA approved a prescription cantharidin formulation for treating molluscum contagiosum, harnessing a vesicant with precision.
Urine therapy and other DIY elixirs

Urine had a long, odd cabinet of uses. Romans valued it for laundering and, in satire and report, for dental whiteness; the chemical sting of ammonia was the workhorse. Some Ayurvedic and tantric texts describe amaroli, or urine therapy, as a regimen. These practices mixed ritual, availability, and a dash of chemistry, though scientific backing for drinking it is lacking.
Ironically, urine did give modern medicine a helper.
In the 1940s, researchers isolated urokinase, a clot-dissolving enzyme, from human urine; refined versions became approved thrombolytics decades later. That is a far cry from do-it-yourself sipping. Contemporary guidelines advise against urine ingestion for health, citing contamination and absence of proven benefit.
Theriac and universal antidotes brewed for centuries

From antiquity to the Enlightenment, apothecaries compounded theriac, a panacea with serpentine lineage. Legends credit Mithridates VI of Pontus with early antidotal recipes; in imperial Rome, physician Andromachus penned a formula featuring opium, aromatics, and even viper flesh, eventually swelling to dozens of ingredients blended and aged.
Entire cities took pride in the brew.
Venice supervised public compounding of its famed treacle, with physicians and notaries overseeing ingredients and timing. English pharmacopeias listed theriac and mithridate into the 18th century before rational pharmacology retired them. With standard doses and controlled trials, fewer ailments demanded a single, spiced catchall.
Tapeworm “treatments” and other parasite-based fixes
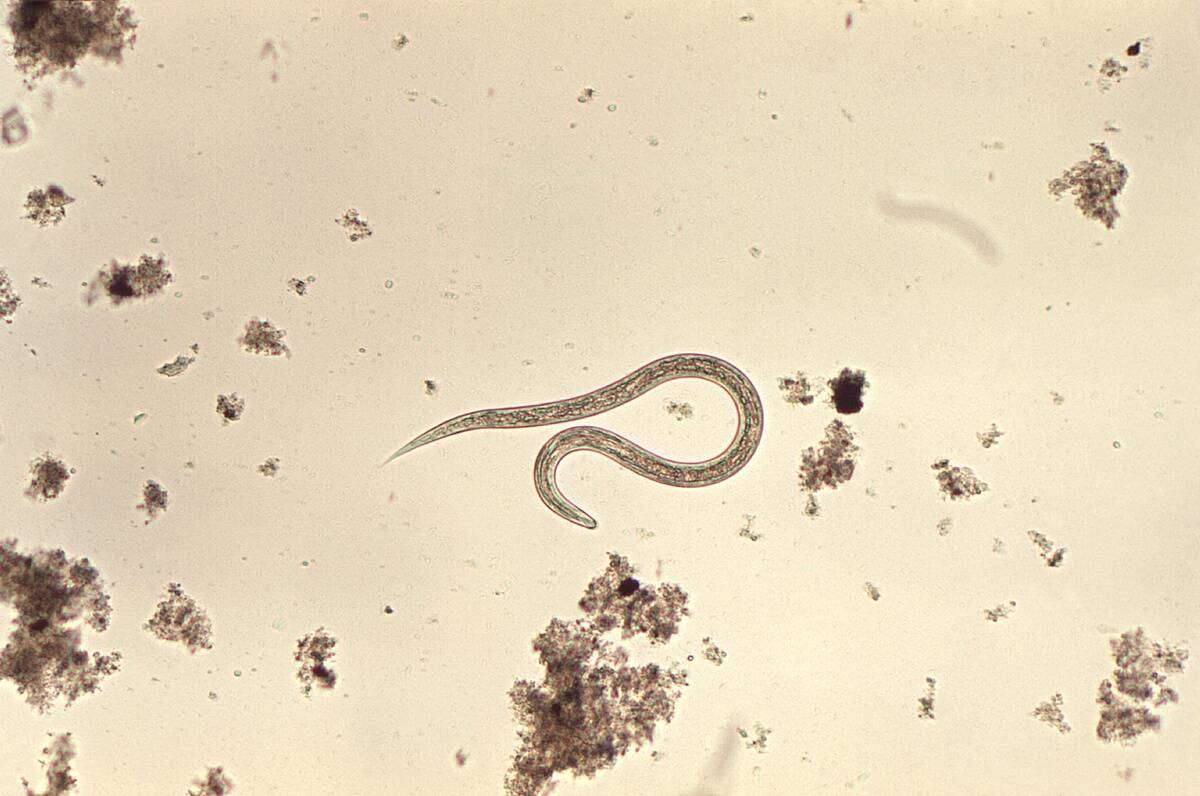
Doctors once fought tapeworms with gusto, not encouragement. Nineteenth-century prescriptions included male fern extract, thymol, and later oil of chenopodium to stun and expel the flat invaders, followed by a purge. It was a messy, sometimes toxic business aimed at recovering the offending scolex to prevent regrowth.
Tales of tapeworm eggs sold for slimming persist, but solid evidence of mainstream medical endorsement is thin; many advertisements look more like stunts or scams. Meanwhile, parasite therapy took a different turn. Sterile maggot debridement, revived in the 1990s, earned FDA clearance in 2004 for chronic wounds. Experimental helminth therapies for autoimmune disease sparked interest in the 2000s, but major trials have not delivered routine care.
X-ray shoe fitters and radium cosmetics: radiation at retail

From the 1920s through the 1950s, shoe stores installed fluoroscopes so customers could watch their toes wiggle inside new oxfords. Trade names like Pedoscope promised perfect fit via X-rays, though repeated exposures added up for clerks and shoppers. As awareness of radiation risk grew, regulators pushed devices out; by the 1970s they were largely gone.
Radiance also hit the vanity case.
In 1930s France, Tho-Radia creams, branded with a Dr. Alfred Curie, touted radium and thorium salts. In wartime Germany, Doramad toothpaste even boasted radioactivity. Once hazards were undeniable, such products vanished, and radiation returned to the hospital under strict shielding.
Electric belts, violet rays, and quack contraptions that buzzed

Electricity felt like bottled lightning in the late 19th century, and entrepreneurs strapped it to everything. Pulvermacher chain belts and Dr. Scott’s electric corsets promised vigor, virility, and relief from neuralgia via mild currents or, sometimes, none at all. Testimonials flowed; peer-reviewed data did not.
Enter the violet ray. These handheld Tesla-coil gadgets sent crackling sparks through glass electrodes to tingle acne, neuritis, and insomnia into submission. For a time they were standard fare in catalogs and parlors. Mid-20th-century actions by the FDA and Federal Trade Commission targeted unsupported medical claims, dimming the neon halo around home electrotherapy.
Kellogg’s enemas, yogurt, and the crusade for the clean colon

At the Battle Creek Sanitarium in Michigan, physician-showman John Harvey Kellogg preached intestinal purity. He prescribed daily enemas, sometimes followed by yogurt administered by mouth and rectum to seed what he believed were friendly bacteria. Guests also got vegetarian fare, exercise, sunbaths, and lectures in a regime that married hygiene with moral zeal. In 1894, John Harvey and his brother Will Kellogg rolled out corn flakes as a plain, digestible food.
Kellogg published extensively, including a 1917 treatise on colon hygiene, railing against autointoxication from sluggish bowels. While his emphasis on fiber, movement, and moderation aged well, the obsession with purgation did not. Still, his sanitarium and cereal empire helped shape modern wellness culture, for better and for bran.
Malaria therapy for syphilis: curing with a fever

Before penicillin, late-stage syphilis was often fatal, especially when it invaded the brain. In 1917, Austrian psychiatrist Julius Wagner-Jauregg induced malaria in patients with neurosyphilis to provoke high fevers that could weaken Treponema pallidum. After several febrile cycles, he treated the malaria with quinine.
The strategy brought measurable recoveries in an otherwise bleak ward.
The risks were real, but in a grim calculus, benefits sometimes outweighed harms. Wagner-Jauregg received the Nobel Prize in 1927 for this work. By the 1940s, penicillin rendered malariotherapy obsolete, offering a safer, simpler cure that did not require trading one pathogen for another.
Cigarettes for asthma: when doctors said “inhale”

In the late 19th and early 20th centuries, pharmacies sold asthma powders and cigarettes made from stramonium (Datura), lobelia, and sometimes tobacco or potassium nitrate. Consumers lit and inhaled the anticholinergic smoke to relax bronchial spasms. Stramonium even appeared in official pharmacopeias of the era as a remedy for asthma attacks, with dosing cautions.
Marketing overreached, and harms mounted. By mid-century, evidence linked smoking with chronic lung disease and cancer, and safer inhaled medicines advanced. The 1964 US Surgeon General’s report cemented the turn against cigarettes. Asthma treatment moved from smoldering paper to metered-dose inhalers and spacers, quietly saving breath without the haze.